The Mommyish Definitive Guide To Infertility: In Vitro Fertilitzation
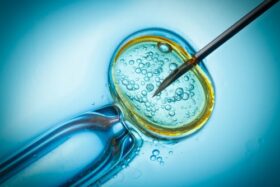 If you’ve undergone fertility treatments in an effort to get pregnant with no luck, at the very bottom of the making a baby via science bag of tricks is In Vitro Fertilization, or (IVF). IVF isn’t typically recommended by doctors without a medical reason until you have exhausted less invasive methods, like medication and Intrauterine Insemination. The IVF process is costly, time consuming and for many, very stressful. This is what it’s like to literally put all of your eggs in one basket when trying to conceive.
If you’ve undergone fertility treatments in an effort to get pregnant with no luck, at the very bottom of the making a baby via science bag of tricks is In Vitro Fertilization, or (IVF). IVF isn’t typically recommended by doctors without a medical reason until you have exhausted less invasive methods, like medication and Intrauterine Insemination. The IVF process is costly, time consuming and for many, very stressful. This is what it’s like to literally put all of your eggs in one basket when trying to conceive.
What is IVF?
Just the facts
Web MD provides a straightforward description of the IVF process. After hormonal treatment to help a woman’s body develop more eggs, the eggs are retrieved. A doctor will combine those eggs with the partner’s sperm and allow them to grow under close observation. When they are ready, they will be put back into the uterus in hopes that they implant and fully develop.
The real deal
If you want to experience pregnancy and not use a surrogate or adopt, IVF is the last stop on the train of advanced reproductive technology. The good news is eggs which are retrieved but not used during the first round of IVF can be frozen for future attempts. If you are open to the idea of increasing your chances for having multiples, your doctor may be willing to transfer more than one embryo at a time.
What’s the success rate for IVF?
Just the facts
Success rates for IVF depend on a number of factors, including the reason for infertility, where you’re having the procedure done, and your age. WebMD puts IVF success rates between 30-40% for women under age 35, with pregnancy rates declining as a woman’s eggs age.
The real deal
The numbers may seem grim, but your doctor will be able to give you a better idea of your chances for success based on your unique set of circumstances. They will also talk with you about how many embryos you want to transfer into your uterus, knowing that doing so increases your chances of having multiples.
Some doctors will recommend a process known as intracytoplasmic sperm injection, or (ICSI) to improve the odds of a sperm fertilizing an egg. In ICSI a sperm is directly injected into an egg in hopes of creating a viable embryo. ICSI may be an additional expense.
There have been studies done about the rate of birth defects in children born using IVF and ICSI. There is continued discussion about whether there is a significant increase in defects with the use of advanced reproductive technology and if any defects among these babies are the result of the procedures used or consequences of underlying fertility issues. Half of the eggs that were harvested for my IVF cycle where fertilized using ICSI and half fertilized naturally. By the day of transfer we had decided to put two embryos in. Of the two healthiest embryos, one was ICSI and one was not. Both embryos resulted in a child without birth defects.
What is the process leading up to the embryo transfer?
Just the facts
Your doctor will give you a medication chart to follow. The medications will likely include injections. The medicine will encourage your body to produce multiple egg follicles at once. You will be monitored via bloodwork and/or transvaginal ultrasound to determine when the follicles are fully developed. When your eggs are deemed ready to be harvested, you will be instructed to give yourself an injection of human chorionic gonadotropin, or HSG, also known as a “trigger shot”. This special injection will cause the follicles to mature and the timing of it must be very precise. The eggs will typically be retrieved 34 to 36 hours after the trigger injection.
The egg retrieval is done with a hallow needle through the vagina with the guide of the transvaginal ultrasound. The woman is placed are under heavy IV sedation during the procedure and afterwards is monitored and given pain medication. Most woman complain of cramping after the procedure.
Your partner will be asked to produce a sperm sample the same day as the egg retrieval, or a previously obtained frozen sperm sample will be thawed. The eggs and sperm will be combined. The lab or doctor’s office will be in touch to let you know how many eggs were retrieved and how they are doing. Depending on the quality of the embryos, transfer will be either 3 or 5 days after retrieval.
If you are doing IVF using frozen eggs or donor eggs, you won’t have to undergo the trigger injection or egg retrieval process. However, you will still need to give yourself a series of injections to prepare your body for the embryo transfer.
The real deal
If you’ve had injectable medications before or underwent an interuterine insemination, you’re probably familiar with needles and medication schedules. IVF medications typically include intramuscular injections, which are given in the thigh or the butt. Some of the medications are suspended in oil, and because the oil is so thick, the pharmacy will give you a wider needle to draw the medication up into the syringe. If you have one of these medications, you must change the needle on the syringe for a smaller one before injecting. The pharmacy will warn you, the doctor will warn you and now I am warning you- DO NOT FORGET TO CHANGE TO THE SMALLER NEEDLE. You will puncture quite the hole in yourself otherwise.
My husband gave me my injections. We used a poke and prod method each night to find a spot on my behind that wasn’t already home to a bruise, but many times we miscalculated. Mommyish commentator Rachel Sea shared her technique last week of doing the injections in a orderly row so that she didn’t inject into damaged tissue. This is a great idea and one I wish I had thought of because the injection was so much worse when it went into muscle that hadn’t healed yet.
Besides leaving painful welts, the injection site may bleed, so have some gauze or cotton pads nearby just in case. Walking for a bit after the shot can help reduce soreness and heating pads are your friend.
Some women feel uncomfortable prior to egg retrieval, as though they are swollen around the ovaries. After egg retrieval many women experience cramps and pain for a couple days. Constipation is another common complaint.
What is the embryo transfer like?
Just the facts
You will be given an appointment time to arrive at the clinic. Because the timing is so precise, it is possible that your transfer will happen on the weekend. It is likely that you will change into a gown (medical, not ball) and will get a medical bracelet with your identification details to match you to your embryos. Usually your significant other is allowed into the procedure room with you. There is no pain medication or sedation for the transfer procedure. A nurse will place an ultrasound wand on your abdomen to allow the doctor to see where the embryos are being placed. Having a full bladder helps make it easier for the doctor to place the embryos into your uterus, so your pre-appointment instructions may include drinking water. The embryos will be retrieved from the lab and safety checks will be performed to make sure you are receiving the right embryos. The embryos will be placed in the uterus using a thin flexible tube called a catheter that is inserted through the cervix. After the procedure they will ask you to lie still for a while and take it easy for a day or two.
The real deal
I wanted to do everything in my power to encourage the IVF to be a success, so I drank a full bottle of water before going in for my procedure. I had so much to drink that while preparing for the transfer, the doctor looked at my bladder via ultrasound and asked if I wanted to pee a little bit before the procedure, because it was so full. I didn’t want to risk over-peeing, so I assured him I was fine, which was a lie. After the procedure, instead of laying calmly and projecting positive thoughts to the embyos in my belly, I repeatedly asked my husband how many minutes had passed because I was dying to go to the bathroom. I lasted 18 minutes out of the doctor recommended 20 before sprinting down the hall to the bathroom. Then I spent another ten minutes squatting over the toilet trying to determine if that teeny black speck in the bowl had just came out of my body and was in fact a dislodged embryo (it was not). Bottom line- drink water if your protocol calls for it, but not too much. And if your doctor suggests you pee beforehand- listen to the person that graduated medical school, they know better than you do on this one.
As for the procedure itself, if you survived the hysterosalpingogram, the embryo transfer is a walk in the park, more uncomfortable than painful, like a PAP smear. I walked into the procedure room and remarked to my doctor that I was disappointing by the lack of roses and mood music. Since he was trying to get me pregnant I would have appreciated a little wooing first.
When it came time to get the embryos, my doctor went over to a window in the wall which opened to the lab and retrieved them from the lab technician. I remember thinking it was just like a drive-through window and having the bizarre impulse to ask him to order me a cheeseburger while he was over there, but I held my tongue.
Despite the occasional story in the news about embryo mix-ups, it was my experience that there are a ton of safety checks to make sure the right embryos go with the right uterus. My medical bracelet was checked several times during the procedure and I had to answer several identification questions when the eggs where transferred from the care of the lab to my doctor. Once the embryos were implanted, my doctor snapped a screen shot of them inside me and labeled it with my medical information as proof of what happened to those particular embryos. We have a copy of that photo, and it’s kind of cool to be able to look back on it and say these little round blobs became my kids.
What happens to any leftover embryos?
Just the facts
Embryos that are not used can be frozen for future rounds of IVF. There is typically an annual storage fee of several hundred dollars to keep embryos frozen. Other options are to have the embryos destroyed, donated towards scientific research or donated to another couple.
The real deal
Our fertility clinic gave us paperwork asking us what we wanted to do with any leftover embryos in detail. It covered all sorts of scenarios- from what our intentions were if one of us were to die, to how we would divide the embryos in the event of a divorce. A hospital won’t do anything with the embryos besides freeze them without the consent of both parties. If you feel overwhelmed trying to make all these choices without knowing if the procedure is going to work, you may be able to mark the situations you are unsure about as “to be determined at a later date.” This was the choice that worked best for me, and after our kids were born we decided to freeze the remaining embryos for a while before ultimately donating them to research.
(image: Shutterstock.com)